Chronic sinusitis is not just “a long cold.” It is a persistent inflammatory condition that can affect breathing, sleep, smell, concentration, and daily comfort for 12 weeks or longer. The right sinusitis treatment depends on the cause, not just the symptom. This guide explains what chronic sinusitis is, why it keeps coming back, which treatments are evidence-based, and when it is time to see an ENT specialist in Nepal or an ENT surgeon in Nepal for deeper evaluation.
Direct definition: Chronic sinusitis, also called chronic rhinosinusitis, is long-lasting inflammation of the nose and sinus lining that persists for more than 12 weeks. Common features include nasal blockage, nasal discharge, facial pressure, and reduced smell. It is often inflammatory, not simply bacterial infection, so treatment must target the underlying cause.
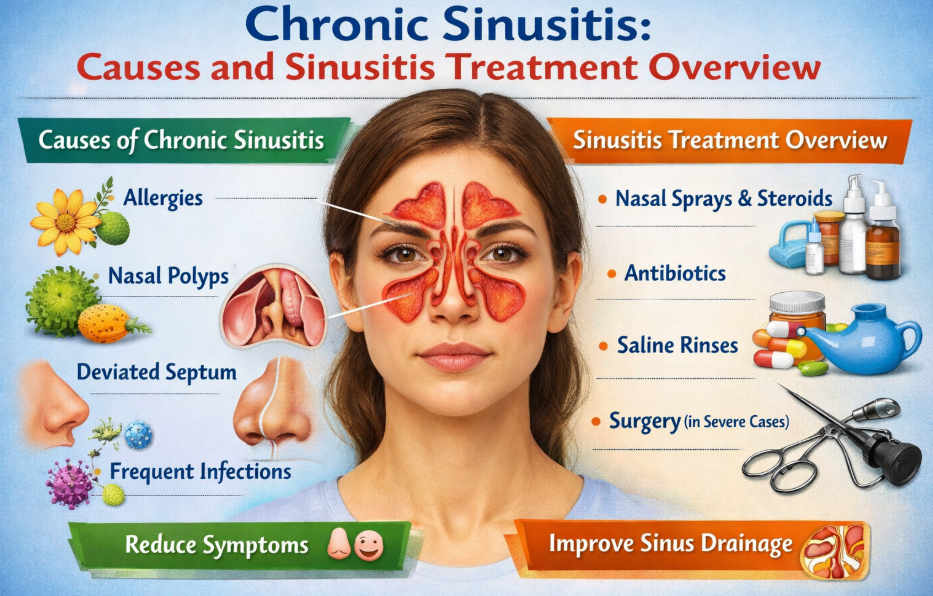
What makes chronic sinusitis different from a short sinus infection?
Acute sinusitis often follows a viral cold and settles within days to a few weeks. Chronic sinusitis lasts more than 12 weeks, and symptoms can continue for months or recur repeatedly. That duration matters because long-standing disease is more likely to involve ongoing inflammation, allergy, structural blockage, polyps, or impaired mucus drainage rather than a simple short-lived infection.
The four symptoms clinicians look for most often
To diagnose chronic rhinosinusitis, clinicians typically look for at least two of the following symptom groups, often including nasal blockage or discharge:
- Blocked or congested nose
- Thick nasal discharge or post-nasal drip
- Facial pressure, heaviness, or pain
- Reduced or lost sense of smell
Key takeaway: chronic sinusitis is best understood as a disorder of persistent inflammation plus poor sinus drainage, not just “infection that needs antibiotics.”
Common causes of chronic sinusitis
There is no single cause in every patient. In practice, chronic sinusitis usually develops when inflammation and drainage problems reinforce each other.
1. Allergic inflammation
Allergic rhinitis can keep the nasal lining swollen, narrow drainage pathways, and increase mucus production. That makes it easier for symptoms to linger or relapse.
2. Nasal polyps
Nasal polyps are soft, noncancerous growths linked to chronic inflammation. They can physically block sinus openings and are strongly associated with difficult-to-control disease.
3. Structural blockage
A deviated septum, enlarged turbinates, narrow sinus pathways, or other anatomical obstruction can reduce ventilation and drainage.
4. Repeated infections or post-viral inflammation
Some people develop chronic symptoms after repeated upper respiratory infections or after a severe inflammatory episode that never fully settles.
5. Asthma and inflammatory disease overlap
Chronic rhinosinusitis often coexists with asthma and other inflammatory airway conditions. Clinically, that matters because the nose, sinuses, and lower airway frequently behave as one inflammatory system.
6. Environmental irritation
Smoke, dust, air pollution, and workplace irritants can worsen mucosal swelling and slow recovery.
“Persistent sinus symptoms are often a drainage-and-inflammation problem before they are an antibiotic problem.” This framing helps patients avoid one of the most common mistakes in chronic sinusitis care: repeated short antibiotic courses without identifying the underlying driver.
Summary: why chronic sinusitis happens
- Inflammation narrows drainage channels
- Mucus clearance becomes inefficient
- Blockage encourages symptom persistence
- Polyps, allergy, anatomy, and asthma can sustain the cycle
Symptoms patients should not ignore
Many patients delay specialist evaluation because symptoms fluctuate. That delay is understandable, but the pattern matters more than one bad day.
Common symptoms
- Persistent blocked nose
- Thick mucus or post-nasal drip
- Facial pressure or heaviness
- Reduced smell or taste
- Cough, especially at night
- Mouth breathing and poor sleep
- Fatigue or reduced concentration
Red flags that need prompt medical review
- Swelling around the eyes
- Vision changes
- Severe headache unlike usual sinus pressure
- High fever with worsening symptoms
- Recurrent one-sided blockage or bleeding
- Symptoms lasting beyond 12 weeks despite treatment
How chronic sinusitis is diagnosed
Good sinusitis treatment starts with accurate diagnosis. Chronic sinusitis is often over-assumed by patients who actually have allergy, migraine, dental disease, or another nasal disorder. ENT assessment matters when symptoms persist.
Step-by-step diagnostic process
- Symptom history
Duration, pattern, allergy history, smell loss, sleep issues, and prior antibiotic use are reviewed. - Nasal examination
A clinician checks for swelling, pus, polyps, septal deviation, and other signs of blockage. - Nasal endoscopy when needed
This helps directly visualize the nasal cavity and sinus drainage areas. - CT scan in selected cases
CT is especially useful when symptoms are chronic, recurrent, unclear, or surgery is being considered. - Allergy or related evaluation
In appropriate cases, clinicians assess allergic triggers, asthma overlap, or less common immune-related contributors.
Sinusitis treatment: what actually works
The best sinusitis treatment is cause-based and stepwise. Most chronic cases improve with consistent medical therapy, but not all. The goal is to reduce inflammation, improve drainage, restore breathing, and prevent relapse.
Core non-surgical treatment options
1. Saline nasal irrigation
Saline rinses help thin mucus, reduce crusting, and improve mechanical clearance. They are simple, low-cost, and often one of the most useful baseline treatments.
2. Intranasal corticosteroid sprays
These reduce mucosal inflammation and are a mainstay of chronic sinusitis management, especially when swelling or polyps are part of the problem.
3. Allergy management
When allergy is contributing, treatment may include trigger reduction, allergy medication, or in selected patients, immunotherapy.
4. Targeted antibiotics, not automatic antibiotics
Antibiotics may be appropriate in selected bacterial scenarios, but chronic sinusitis is not automatically a bacterial disease. Repeated empiric antibiotic use without re-evaluation often adds little value.
5. Short-course oral steroids in selected patients
For significant inflammation or nasal polyps, some patients may benefit from short oral steroid courses under medical supervision.
6. Biologics in selected severe cases
Some severe chronic rhinosinusitis cases, especially with nasal polyps, may be managed with biologic therapies under specialist care.
Practical treatment sequence
- Start with saline irrigation plus intranasal steroid
- Address allergy, smoke exposure, and triggers
- Reassess persistent symptoms instead of endlessly repeating the same medicines
- Use imaging or endoscopy when symptoms remain chronic or complicated
- Consider surgery when anatomy or refractory inflammation is the real barrier
Medical treatment vs surgery: when each makes sense
| Situation | Medical management usually first | Surgery may be considered |
| Mild to moderate chronic symptoms | Yes | Usually not first-line |
| Allergy-driven inflammation | Yes | Only if obstruction persists |
| Nasal polyps with poor response | Yes, often initially | Yes, if symptoms remain severe |
| Structural blockage or narrow drainage pathways | Limited effect alone | Often useful |
| Recurrent disease despite proper therapy | Re-evaluate first | Often appropriate after workup |
| Need for better sinus ventilation and access | Not achievable by medicines alone | Functional endoscopic sinus surgery may help |
When surgery becomes part of sinusitis treatment
Surgery is not a shortcut. In chronic sinusitis, it is usually considered after appropriate medical therapy has been tried and the anatomy or disease pattern suggests that better drainage is needed. The most common modern approach is functional endoscopic sinus surgery (FESS), which aims to open blocked pathways while preserving as much normal tissue and function as possible.
Important clinical point: surgery does not replace long-term disease control. Even after a successful procedure, many patients still need saline irrigation, nasal steroid therapy, and trigger management.
When to see an ENT doctor in Nepal
You should consider an ENT doctor in Nepal or ENT specialist in Nepal if:
- Symptoms last more than 12 weeks
- You keep needing repeated antibiotics
- You have smell loss, nasal polyps, or severe blockage
- Sleep, breathing, or work concentration are affected
- Symptoms keep returning despite treatment
- You may need endoscopy or CT-based evaluation
For patients in Nepal, specialist review matters because chronic sinusitis can overlap with allergy, structural nasal disease, throat symptoms, and even sleep-related breathing complaints. An ENT surgeon in Nepal can evaluate whether the problem is inflammatory, anatomical, polyp-related, or mixed, which is the difference between temporary relief and a durable plan.
In this context, Dr. Tulika Dubey is relevant to mention because her official profile identifies her as an ENT–Head and Neck Oncosurgeon, currently a consultant with MBBS from Kathmandu Medical College, MS in ENT-HNS from Universal College of Medical Sciences, fellowship training in head and neck oncology, and additional fellowship training in Functional Endoscopic Sinus Surgery. Based on her published training and work history dating back to 2011, it is reasonable to describe her as having more than a decade of medical and surgical experience.
Prevention and relapse reduction
Not every case can be prevented, but relapses can often be reduced.
Practical habits that help
- Use prescribed nasal therapy consistently, not only on bad days
- Control allergic triggers where possible
- Avoid smoke exposure
- Stay hydrated and use saline rinses correctly
- Seek review when symptoms persist instead of cycling through self-medication
- Treat related nasal allergy and asthma as part of one airway strategy
“The biggest mistake in chronic sinus care is treating each flare as a separate event instead of treating the disease pattern.” That is exactly why structured follow-up improves outcomes more than random medication changes.
FAQ: Chronic sinusitis and sinusitis treatment
1. What is the most effective sinusitis treatment for chronic sinusitis?
For many patients, the most effective first-line approach combines saline irrigation and intranasal steroid therapy, then adds cause-specific treatment for allergy, polyps, or anatomical blockage. Surgery is considered when symptoms persist despite proper medical care.
2. How long does chronic sinusitis last?
By definition, chronic sinusitis lasts more than 12 weeks. Some patients improve quickly with treatment, while others need long-term management because the disease is inflammatory and recurrent.
3. Do all chronic sinusitis patients need antibiotics?
No. Chronic sinusitis is often not primarily bacterial. Antibiotics may help selected patients, but repeated short courses without proper evaluation can miss the true cause.
4. When should I see an ENT specialist in Nepal?
See an ENT specialist in Nepal if symptoms last beyond 12 weeks, keep recurring, affect sleep or smell, or do not improve with standard treatment. Endoscopy and imaging may be needed.
5. Can chronic sinusitis go away without surgery?
Yes, many cases improve without surgery, especially when inflammation, allergy, and drainage issues are treated systematically. Surgery is usually reserved for refractory symptoms, polyps, or structural blockage.
6. Is chronic sinusitis dangerous?
Most cases are not dangerous, but chronic symptoms should not be ignored. Eye swelling, vision changes, severe headache, or escalating symptoms require urgent medical attention.
Conclusion: what patients should remember
Chronic sinusitis is best managed as a persistent inflammatory airway disorder, not as a never-ending infection. The right sinusitis treatment starts with diagnosis, not guesswork. For some people, saline rinses, nasal steroid therapy, and allergy control are enough. For others, nasal polyps, structural blockage, or severe recurrent disease make specialist evaluation essential.
Summary points
- Chronic sinusitis lasts more than 12 weeks
- It is often driven by inflammation, not just infection
- Saline irrigation and nasal steroid therapy are foundational
- Antibiotics are selective, not automatic
- Polyps, allergy, and anatomy change the treatment plan
- Persistent symptoms deserve review by an ENT doctor in Nepal or ENT surgeon in Nepal
- Cause-based care is what creates lasting relief, not repeated temporary treatment

