Transformational Head & Neck Cancer Care in Nepal
If you’re looking for a trusted Head & Neck Oncosurgeon in Nepal, you’re in the right place. I’m Dr Tulika Dubey, an ENT and Head & Neck Oncosurgeon practising in Nepal, dedicated to delivering compassionate, advanced care for patients facing the toughest Head & Neck Cancer diagnoses. Whether you or a loved one are grappling with a tumour of the throat, salivary glands, thyroid, or other head/neck region, this post will walk you through what head & neck oncosurgery involves, how to recognise early signs, what to expect from treatment and how to partner with the right surgeon.
Let’s begin your next chapter understanding your condition, addressing your concerns and making empowered decisions for your care.
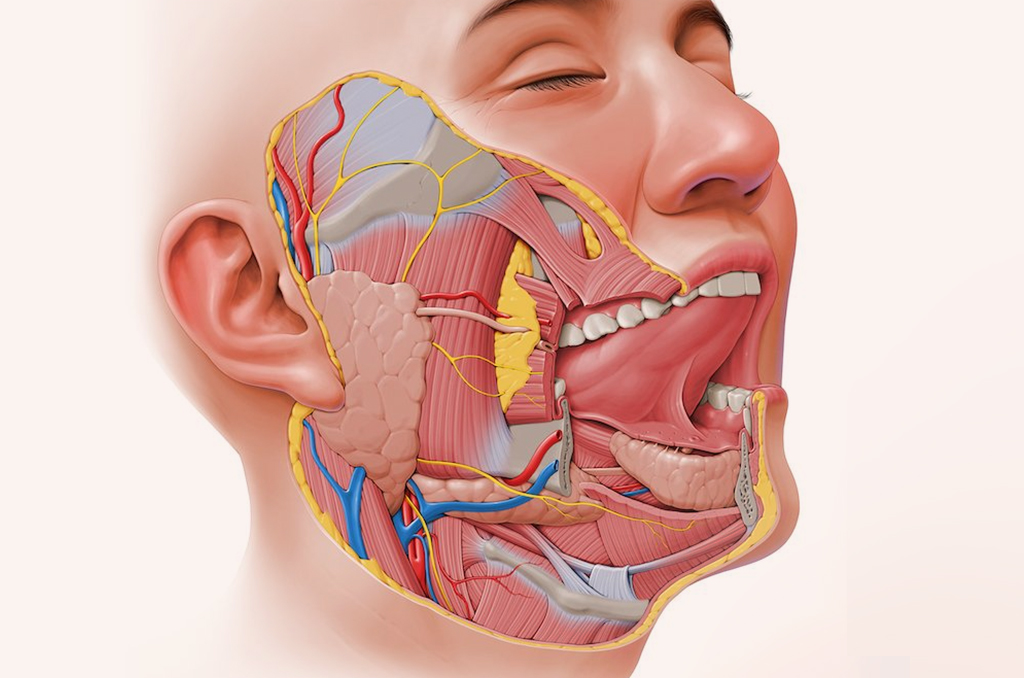
1. What Does an ENT Head & Neck Oncosurgeon Do?
As a specialist in the head/neck region with training in ENT and oncology, I handle both benign and malignant conditions affecting the face, neck, throat and related anatomy.
Here’s what this care involves:
- Diagnosis: Identifying tumours of the thyroid, salivary glands (parotid, submandibular), oral cavity (tongue, floor of mouth), larynx (voice box), nasopharynx, and other head/neck sites.
- Surgical treatment: From minimally invasive removal of small lumps to complex resections and reconstruction, sometimes with microsurgical techniques.
- Multidisciplinary care: Working in conjunction with radiology, pathology, radiation oncology, medical oncology and reconstructive surgery to craft a personalised plan.
- Rehabilitation & follow‑up: After surgery we focus on helping you recover swallowing, speech, voice, appearance and monitor for recurrence or complications.
In Nepal, choosing a true Head & Neck Oncosurgeon in Nepal matters because the anatomy is complex, the reconstruction needs are unique, and the regional context (resources, patient factors, environment) differs from many other places.
2. Recognising Early Signs: What to Look Out For
Early detection often leads to better outcomes. If you or someone you know has any of the signs below, it’s worth consulting a specialist early.
Signs & Symptoms
- A persistent lump or swelling in the neck or under the jaw, especially if it’s hard, growing, or fixed.
- A sore throat or discomfort in the throat that lasts for more than a few weeks, especially when swallowing gets harder.
- Hoarseness or a change in voice that doesn’t resolve with usual treatment.
- A long standing ulcer or wound inside the mouth that isn’t healing and may bleed easily.
- Blood in saliva or sputum without other clear cause.
- Swelling or pain in the salivary glands area (near ear/cheek) or facial nerve weakness near the parotid gland.
- Persistent ear pain, ear discharge, or hearing loss combined with other head/neck symptoms.
- Thyroid nodules that grow, become hard, stuck to surrounding tissues, or are associated with voice change.
Bear in mind: These symptoms don’t always mean cancer but they do warrant prompt evaluation by a qualified specialist.
3. Understanding the Treatment Journey
Undergoing treatment for head & neck conditions can feel overwhelming. My aim as your Head & Neck Oncosurgeon in Nepal is to guide you step by step with clarity, compassion and expertise.
a) Pre‑operative Consultation
- We review your symptoms, medical history, imaging and biopsy reports as needed.
- We explain your diagnosis in plain language: what it means, urgency, treatment options, expected benefits and risks.
- We discuss cost, recovery time, likely outcomes and your personal concerns.
- We ensure you’re comfortable and informed, not rushed.
b) Surgical Intervention
- Surgery might range from removal of a small tumour (with minimal impact) to complex resections including bone, soft tissue, nerve reconstruction, etc.
- We always aim for organ preservation when feasible: preserving the voice box, swallowing mechanism, appearance.
- I coordinate with reconstructive and rehab specialists to maximize your functional and cosmetic outcome.
c) Post operative Care & Rehabilitation
- You’ll receive instructions on wound care, diet progression, pain and infection control.
- If voice or swallowing are affected, early therapy is crucial (speech/swallow rehab).
- Follow ups will monitor healing, function and readiness for any additional treatments like radiation or chemotherapy.
d) Long Term Follow‑Up
- Head & neck cancers have unique recurrence risks so consistent monitoring is essential.
- Lifestyle modification plays a big role in long‑term success.
- Some effects (voice changes, swallowing issues, appearance) may improve over months. Rehab and patience are key.
4. Common Head & Neck Oncosurgical Conditions I Treat
Here are some of the frequent conditions I handle, so you can see whether your situation aligns.
- Thyroid cancer or suspicious thyroid nodules: Rapid thyroid growth, change in voice, hard nodes.
- Salivary gland tumours (parotid, submandibular): Swelling near ear/jaw, pain, facial nerve involvement.
- Oral cavity & tongue cancers: Persistent ulcers, red/white patches, abnormal bleeding.
- Laryngeal (voice box) cancer: Prolonged hoarseness, throat pain, breathing difficulty.
- Nasopharyngeal / oropharyngeal cancers: Ear fullness, nasal obstruction, neck masses.
- Skin cancers of the head/neck region: Changing moles, non‑healing lesions on face/neck that bleed or ulcerate.
- Recurrent head/neck tumours or second primary cancers: Patients previously treated who now need further specialised care.
As your dedicated Head & Neck Oncosurgeon in Nepal, I bring focused experience in these areas, not a general ENT procedure list.
5. Why Choosing the Right Surgeon & Clinic in Nepal Matters
What to look for:
- Specialisation: Ensure the surgeon is trained specifically in head & neck oncology, not just general ENT.
- Multidisciplinary team: Access to radiology, oncology, reconstructive surgery and rehabilitation under one roof.
- Modern infrastructure: Advanced imaging, operating theatre facilities, endoscopic/laser equipment, reconstructive capabilities.
- Transparent communication: The clinic should discuss condition, plan, cost, risks and expected outcomes clearly.
- Patient‑centred approach: You should feel listened to; your voice, swallowing, appearance and quality of life matter.
- Aftercare & follow‑up: Treatment is not finished when you leave surgery, you’ll need monitoring, rehab program and support.
In the Nepal context; where geography, resources, patient access vary, choosing a clinic led by a dedicated Head & Neck Oncosurgeon in Nepal ensures your care is geared to local realities and best practices.
6. Lifestyle & Recovery: What You Can Do to Improve Outcomes
Your active participation matters. These lifestyle steps complement your care with a head & neck specialist:
- Quit smoking & limit alcohol: These are major risk factors for head & neck cancers and recurrence.
- Nutrition: After surgery you’ll need lean protein, fresh fruits/vegetables, whole grains and good hydration to heal promptly.
- Protect your skin & neck: Use sun protection, avoid excessive sun‑exposure, protect your face/neck if you work outdoors.
- Voice/swallow rehab: Engage early with therapy if your surgery affected voice or swallowing. Delaying therapy may reduce recovery.
- Exercise & posture: Gentle walking, breathing exercises and neck/shoulder mobility help especially if you’ve had neck dissection.
- Follow up vigilance: Attend all appointments, report any new lumps, hoarseness or swallowing changes immediately.
- Emotional/psychological support: A diagnosis in the head & neck region affects not only health but identity (voice, appearance). Seek counselling or join support groups if you feel isolated.
With your surgeon’s expertise, your commitment and a supportive team, you’ll be positioned for the best possible outcome.
7. Frequently Asked Questions (FAQ)
Q: How soon should I consult a head & neck specialist if I find a lump in my neck?
A: Sooner rather than later. A lump lasting more than 2‑3 weeks, especially if hard/fixed, justifies evaluation. Early diagnosis often means less invasive treatment and better recovery.
Q: Will I lose my voice or ability to swallow after surgery?
A: Not necessarily. Many modern procedures aim to preserve voice and swallowing function. Some may need therapy after surgery. Full recovery is absolutely possible with the right team.
Q: What are the risks of head & neck surgery?
A: As with any surgery: bleeding, infection, wound issues. Specific to head & neck: changes in voice, swallowing, sensation, appearance. We will discuss all risks thoroughly before treatment.
Q: Can head & neck cancer be prevented?
A: Some risk factors like smoking, alcohol, HPV, sun exposure are modifiable. Regular check‑ups, prompt evaluation of symptoms and healthy lifestyle help reduce risk.
Q: Why choose a dedicated Head & Neck Oncosurgeon in Nepal rather than a general surgeon?
A: Because head & neck anatomy is complex and surgery affects critical functions (voice, swallowing, breathing, appearance). A specialist brings focused training, experience and a team to manage all aspects, especially in Nepal where resources may differ.
Summary
Your journey through head & neck cancer care is deeply personal but you don’t have to walk it alone. With the right specialist by your side, one who understands the anatomy, the reconstruction, the local context and your individual goals you can face this challenge with confidence and hope.
If you’re looking for compassionate, expert care from a head & neck specialist in Nepal who will see you, your voice, your future .Let’s work together. You deserve to live well, to speak, to eat, to shine.
Warm regards,
Dr Tulika Dubey,
ENT‑Head & Neck Oncosurgeon, Nepal

